Navigating the world of healthcare billing can be a tumultuous ride. Below are six CentralReach billing features you can implement NOW to easily get your claims processed faster and more efficiently!
Client and Payor Setup.
Are your claim forms having the information you want in the boxes you want? This sounds easy, it’s information in a box, but setup helps ensure that your data is coming to you or your billing team as complete as possible. You can default client Diagnosis codes, boxes (and their digital equivalents) 17, 31, 32, 33, all within CentralReach. Pointers and modifiers can also populate the boxes for you as well!
If you are having incomplete data dropped to your billing entries, then that can create incomplete claims. Be an investigator: investigate the source(s) of the problem, and get that data backfilled. Each area of “drop in” in CR is mapped to a location. Go back to that place, and fill it in. Usually, we tell clients, that with proper setup, within 2 batches or so, you can get almost all of the data setup to be trouble free, because dropping the data to claims should be the fastest part of the claims process.
ERA.
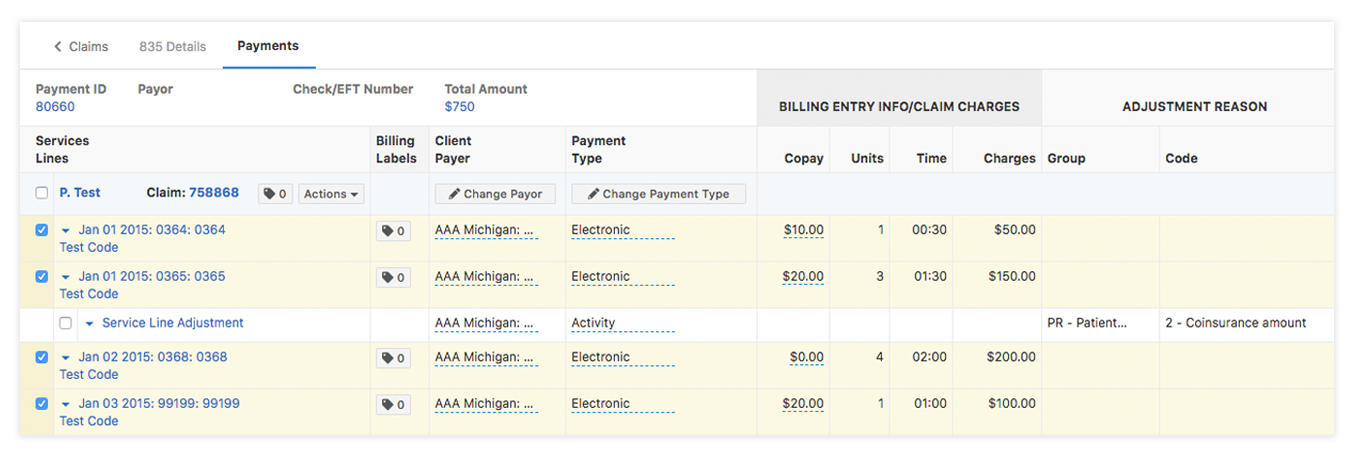
ERAs (Electronic Remittance Advice) are just digital versions of paper EOBs (Explanation of Benefits). Just, we know, right? They are amazing. Since an ERA is coded and standardized, just like an outgoing claim, having a system that can read the ERA data is amazingly fast and easy to use. Now, this does not mean that an insurance payor, paid you correctly, but it is a fantastic tool to post all the itemized payment data, to the itemized billing entries, and that is what claims are all about, itemized entries. The pain here for most companies is how to read and post this data quickly and accurately. In order to take advantage of ERAs, you must submit electronically via CR, and the ERA must come back to CR from the clearinghouse as well. Make sure that you take advantage of this, and if needed, sign up with your payors to use this service that they already offer (in most cases).
Secondary Claims.
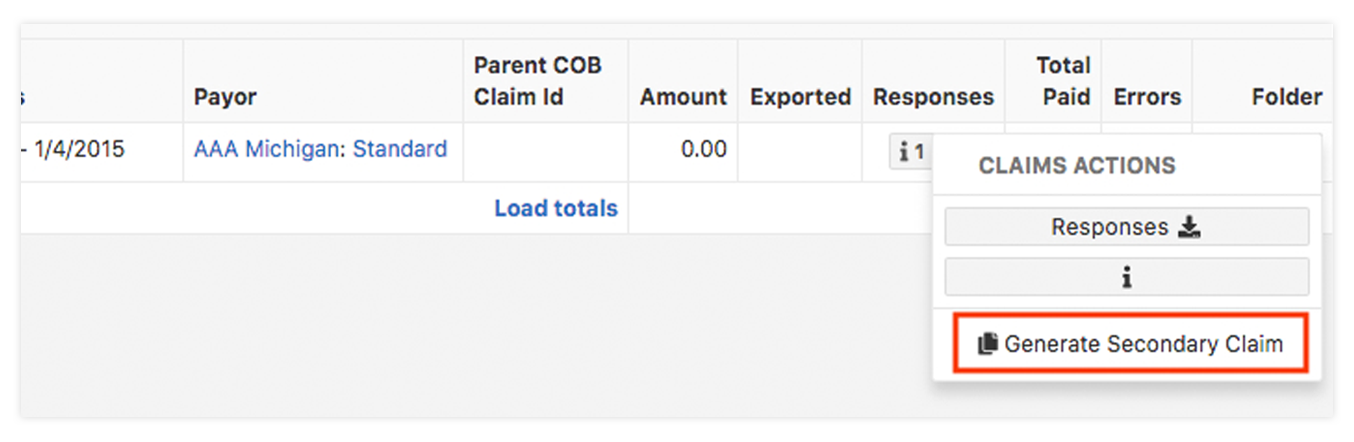
Billing secondary is difficult, no matter how you slice it. Paper secondary claims can be made in CR easily, especially if all the payor info is set up for all payors that belong to a client. Some payors even offer secondary electronic claims– check your clearinghouse to see which ones offer it. If so, CR is now able to send secondary claims electronically as well. The one thing you will need to ensure though, is that you are receiving the ERAs from the primary payor(s). The reason for this is so that CR can capture and transmit all of the ANSI coded payment information with the secondary claim(s).
Invoicing.
When it comes time to invoice your clients, copay (patient responsibility), or self/private pay, as long as you have the data in all the right boxes it can be a snap. Using the filters on the billing screen you can select a large date set, then filter to only outstanding items (money to be collected!). This will pull all entries that show an amount owed, and leaves all zero owed amounts behind. Then you can generate up to 5000 lines of data to invoices at once. Also, if you know what copay is owed we are seeing more and more organizations billing copays right after they bill insurance.
Frequency.
What I mean by this is your billing cycle. Many people think that this is dictated by your employees converting their appointments. While that is still our number one complaint (yes, we wish we could make people convert as well), remember it is up to you to determine your billing timelines, and enforce them. There are tools in CR to have the system look at the schedule and find any unconverted appointments. So, admin team, set your dates and start contacting employees who have not converted. If you like to export data, then run the export, make a HIPAA compliant format from the data, and email out as needed.
Billing screen tools.
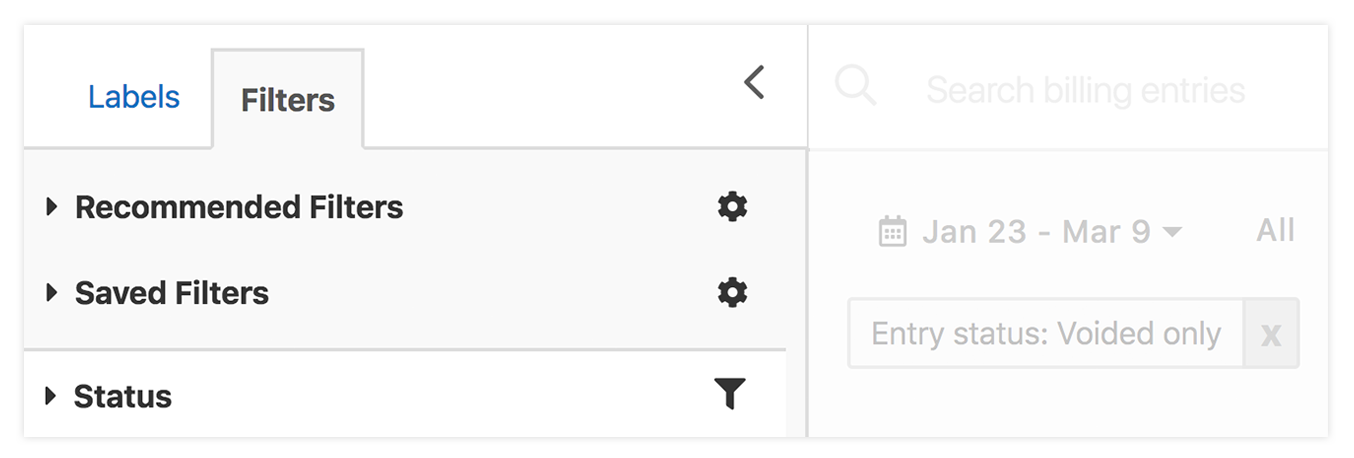
There are lots of ways to filter data, but you do not have to be limited by only the data you see on the screen. Remember you can use your contact labels, service code labels, billing entry labels, etc. Since these are all custom defined you can define your workflow to best suit your needs. Also, have you ever looked at and played with all the filters on the billing screen, there are many, check them out!
Lastly, if you are having trouble billing and getting paid, check out our preferred vendors’ page. We also have a great recorded webinar walking you through CentralReach’s Billing module, for your viewing pleasure.
About the author: Adam Sellers is a CentralReach Billing and Practice Management subject matter expert working from Utah.




