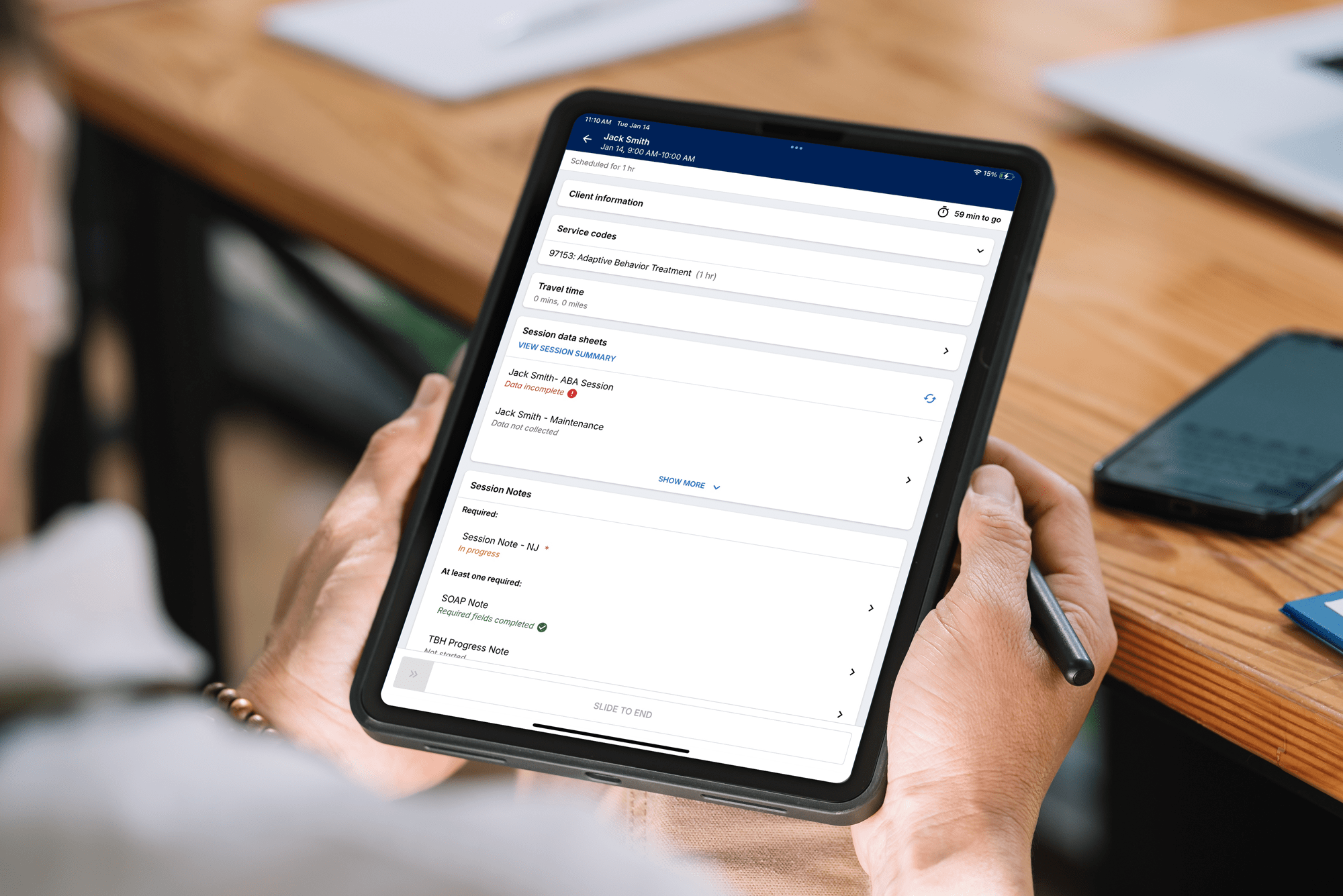
In many ABA organizations, billing delays don’t start in the billing department. They start with late session notes.
When documentation is delayed, the entire revenue cycle slows down. Billing teams can’t confidently submit claims without the documentation needed to validate the service delivered. As a result, supervisors and administrative staff often spend valuable time chasing down technicians to complete notes instead of focusing on higher-value clinical and operational work.
Timely session notes are an operational priority. When documentation lags behind care delivery, billing slows, administrative workload increases, and audit risk grows. That’s why many organizations are rethinking how documentation happens. Instead of writing notes at the end of the day or days later, forward-thinking teams are adopting mobile-first documentation workflows to help clinicians capture session details closer to the point of care.
Why Documentation Timeliness Matters for Billing
Documentation timeliness is a billing issue, not just a clinician habit. Before a claim can be submitted, billing teams need to verify that the services delivered are properly documented. That means having accurate, complete session notes available for review.
Once a session note is submitted, billing teams can review the documentation to confirm the service details and ensure the claim is supported before submission. When notes are completed at the end of a session or shortly afterward, this review can happen sooner, allowing claims to move through the revenue cycle more efficiently.
Delayed notes, however, create operational bottlenecks and increase administrative burden. Staff often have to track down technicians, follow up on missing documentation, or clarify incomplete details before claims can move forward. Each additional step slows the billing workflow.
Three Layers of Risk: The Real Cost of Delayed Session Notes
The cost of delayed documentation goes beyond minor inconvenience. When session notes aren’t completed promptly, the effects ripple across an organization’s operations, impacting revenue cycle performance, compliance readiness, and clinical oversight.
When sessions are delivered but not yet documented, services begin to pile up in a “not billable yet” backlog. Billing teams can’t submit claims until the supporting documentation is completed, resulting in stagnant cash flow.
Delayed notes can also contribute to denied claims. In some cases, timely filing deadlines may approach before documentation is finalized. In others, incomplete or insufficient documentation may fail to support the billed service, leading to denials or additional requests for information.
These scenarios create additional work for administrative teams, who must track down missing notes, correct errors, and resubmit claims, adding unnecessary labor to the revenue cycle.

Why Late Notes Happen (Hint: It’s Usually the Workflow)
If timely session documentation is so important, why do late notes remain such a common challenge for many ABA organizations? For most, the problem isn’t motivation; it’s workflow friction. The way sessions are delivered and the way documentation is managed don’t always align.
Here are a few of the most common causes of late session notes.
1. Unreliable Connectivity in Real-World Settings
ABA providers often work in environments where Wi-Fi is unavailable or inconsistent. When documentation systems require an internet connection, technicians may have to wait until later in the day to complete their notes.
2. End-of-day “Note Marathons”
After a full day of back-to-back sessions, the last thing technicians want to tackle is a backlog of documentation. When barriers prevent notes from being completed immediately after a session, the work tends to pile up at the end of the day.
Over time, this creates the dreaded “note marathon,” where technicians must write multiple session notes at once. This process can be time-consuming and mentally taxing, making it more likely that documentation will be delayed or pushed to the next day.
3. Paper-First Data Collection
Some providers still collect session data and notes on paper before transferring that information into their ABA software later. This duplicate process adds unnecessary administrative work and increases the risk of human error. It also creates a delay between when care is delivered and when documentation is finalized.
4. Tools Designed for Desktops, Not Point-of-Care
Many practice management and clinical data collection platforms were originally designed for use in controlled environments, like an office. As a result, they can be inefficient to use while delivering services in homes, schools, and the community.
Even in clinic environments, clinicians are rarely stationary. They spend most of their time actively engaged in sessions rather than sitting at a computer. When documentation tools are designed primarily for desktops, clinicians often have to postpone writing session notes until the end of the day—or even later.
5. Inconsistent Templates and Unclear Expectations as Teams Scale
As organizations grow, documentation practices can become inconsistent without clear standards in place. Technicians may spend extra time trying to determine what information should be included in a note or how it should be structured. This lack of standardization slows documentation and can lead to incomplete or inconsistent records.
When these workflow barriers exist, even highly motivated clinicians may struggle to keep documentation timely. The result is a higher likelihood of late note submissions, as well as inaccuracies and missing details.

What “Timely” Looks Like in a Scalable ABA Operation
Timely documentation is key, but what does that look like in a growing practice? As organizations expand, maintaining consistent documentation across larger teams becomes more complex. Clear expectations and structured workflows help ensure that session notes support both clinical care and billing operations.
In practice, timely documentation should:
Be completed as close to the point of care as possible.
Ideally, notes are finalized the same day as the session. Capturing session details during the session or shortly afterward helps preserve accuracy and allows services to move through billing review without unnecessary delays.
Include standardized required fields.
Structured templates ensure clinicians capture the information needed to validate the service delivered. This reduces the likelihood of missing documentation elements that could slow claim submission. Features like auto-populated fields, dropdown menus, and checkboxes also simplify the process and reduce the amount of manual entry required.
Allow supervisors to quickly identify trends.
Notes should be submitted soon enough for supervisors to review session outcomes and identify patterns. When documentation is timely, supervisors can provide feedback sooner and make adjustments to treatment plans.
Support both clinical oversight and payor requirements.
Well-structured session notes should clearly reflect what occurred during the session while also including the elements required to support billing and withstand potential audits.
From End-of-Day Notes to Real-Time Documentation
To reduce delayed session notes and the billing delays that often follow, many ABA organizations are shifting to mobile-first documentation workflows. Instead of writing notes at the end of the day or days after a session, mobile tools allow clinicians to capture session data and key details in real time, wherever services are delivered.
With mobile documentation apps that include offline functionality, technicians can document sessions even when internet access isn’t available. Once connectivity is restored, notes can sync automatically, allowing clinicians to complete documentation during or immediately after a session without worrying about connectivity barriers.
AI-powered documentation tools can further support timely documentation. AI-assisted session narratives help organize session data into structured notes, significantly reducing the time required to complete documentation. By easing the administrative burden, these tools make it easier for technicians to finalize notes promptly while maintaining clinician oversight and accuracy.
Document Sessions Closer to the Point of Care
With mobile documentation apps that include offline functionality, technicians can document sessions even when internet access isn’t available. Once connectivity is restored, notes can sync automatically, allowing clinicians to complete documentation during or immediately after a session without worrying about connectivity barriers.
AI-powered documentation tools can further support timely documentation. AI-assisted session narratives help organize session data into structured notes, significantly reducing the time required to complete documentation. By easing the administrative burden, these tools make it easier for technicians to finalize notes promptly while maintaining clinician oversight and accuracy.
Posted in Clinical, Practice Management
You may also like...
Related information and stories
The Consequences of Inconsistent Documentation in ABA
In ABA therapy, documentation serves multiple purposes. It’s necessary for progress monitoring and clinical decision-making. It’s also essential for validating medical necessity and ensuring practices meet payor and regulatory requirements. Clear and consistent documentation is a…
How Swann Clinic Improved Session Note Quality and Cut Documentation by Up to 50%
Swann Clinic for Behavioral Health, a mid-size, multidisciplinary provider in Colorado, needed a more efficient way to maintain consistent documentation across its six locations. For mid-size ABA providers, scaling up…
Leveraging AI for Note Generation To Manage the Complexities of ABA Session Notes Compliance & Audits
ABA providers are under increasing pressure to get documentation right as payors become more stringent in their expectations. Insufficient supporting documentation is one of the most common reasons for failing…