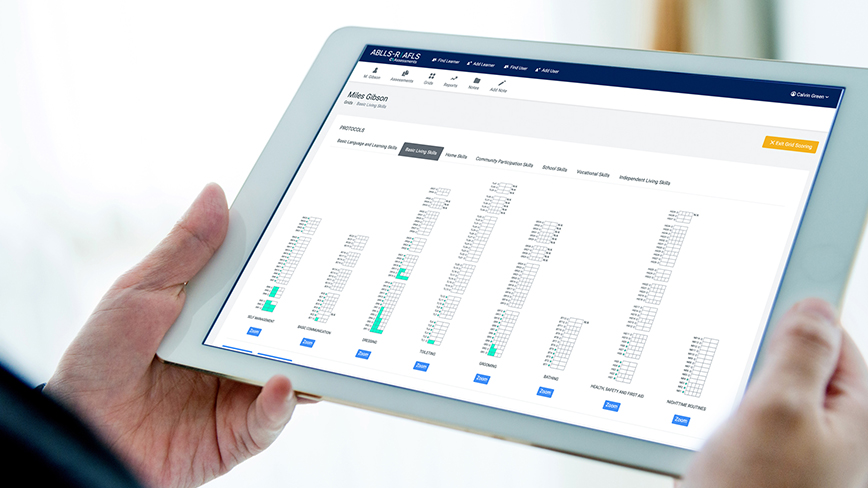
Assessment is foundational to autism and IDD care. It shapes how clinicians understand a learner, identify goals, determine treatment intensity, and measure progress over time. Yet in practice, traditional approaches often fall short, failing to deliver standardized, actionable insights that meaningfully guide care.
At the same time, expectations across the field are changing. Clinicians, providers, and payors are placing greater emphasis on measurable progress, individualized care, and accountability. This shift has exposed a critical gap: the tools and workflows used to evaluate learners aren’t always designed to support the dynamic, data-informed care the field now expects. To move forward, assessment must evolve from a static requirement into a continuous driver of clinical decision-making.
This challenge has been a central focus of recent research and industry efforts to improve the measurement of outcomes in autism care. Dr. Thomas Frazier, Chief Clinical Officer at CentralReach and the visionary behind AI.Measures (AIM), brings decades of clinical, research, and leadership experience to this work. A licensed clinical psychologist, former Chief Science Officer and current national board member at Autism Speaks, and former director of the Cleveland Clinic Center for Autism, Dr. Frazier has spent over 20 years developing and validating assessment tools that support evaluation and treatment. His work has consistently emphasized a critical gap in the field: assessment is too often disconnected from real-world care. Through his research, publications, and national contributions, he has been at the forefront of advancing approaches that better support clinical decision-making, track meaningful progress, and ultimately improve outcomes.
The Disconnect Between Assessment and Treatment
Despite its central role, assessment is often disconnected from subsequent steps in the care process. In many cases, it becomes a task completed to satisfy payor requirements for authorization. Findings are documented, submitted, and repeated every six months, but not consistently used to guide ongoing treatment decisions.
Part of the issue lies in the way many traditional assessment approaches function in practice. While widely used and clinically valuable, many were not designed to support ongoing intervention. Results often require complex interpretation and don’t easily translate into treatment goals, teaching strategies, or day-to-day clinical decisions.
There are also structural limitations. Many assessments serve as one-time snapshots, offering limited insight into how a learner is progressing over time. Without a clear connection between results and intervention, clinicians are left without the insight needed to confidently adjust care or demonstrate outcomes.
In addition, these approaches often fail to account for the wide variability across learners. Differences in behavioral challenges, developmental trajectory, and co-occurring conditions can significantly impact progress, yet many assessment models don’t adjust for these factors, making it difficult to interpret outcomes accurately or fairly.
Assessment processes can also lack standardization, be time-intensive, and prone to error, particularly when workflows are fragmented, placing additional burden on clinicians while limiting clinical utility. As highlighted in Dr. Frazier’s research and recent contributions to the Department of Defense’s Autism Care Demonstration Program, this disconnect isn’t just a workflow issue. It reflects a broader gap between how assessment is conducted and how care is actually delivered.
Rethinking the Role of Assessment in Autism and IDD Care
If assessment is going to meet the demands of modern autism and IDD care, it must move beyond static evaluation and become an active part of the clinical process. Rather than serving as a one-time requirement, assessment should function as a continuous guide, informing what to teach, how to teach it, and when to adjust course.
Clinicians should be able to answer critical questions throughout care:
- Is the learner making meaningful progress?
- Do goals and interventions need to change?
- Is the current level of care appropriate?
This shift requires more than better tools. It requires a different approach to measurement. Assessment must connect directly to treatment, translate results into clear next steps, and support ongoing, data-informed decision-making. It must also move beyond static reporting to provide ongoing insight into whether interventions are producing meaningful, reliable change.
What Modern Assessment Should Deliver
For assessment to truly support clinical care, it must do more than evaluate. It must actively inform what happens next.
A comprehensive view of the learner
Modern tools should capture the full range of skills and challenges that impact daily life. Criterion-referenced assessments like ABLLS-R and AFLS play a critical role here, offering structured frameworks to evaluate language, learning, and functional living skills. These tools help clinicians move beyond surface-level insights to understand what truly matters for independence and quality of life.
A direct connection to treatment
Assessment results should translate into actionable treatment plans. Skill-based frameworks like ABLLS-R and AFLS are particularly valuable because they break down complex abilities into teachable components, making it easier to identify targets, build goals, and guide instruction.
Built-in progress tracking
Assessment should not function as a one-time event. Clinicians need to track change over time and determine whether progress is meaningful, not just observable. More advanced approaches, including multi-modal measurement models like AIM, help integrate multiple data sources to provide a clearer, more reliable picture of outcomes. This approach adds value by helping to synthesize multiple data sources and reporting progress using the most sensitive methods for monitoring improvement.
Contextualized, individualized insight
Modern measurement should account for differences in learner profiles, including the attributes of the learner and an individualized expectation about the rate of progress. This ensures that outcomes are interpreted accurately and supports more equitable, data-informed care decisions.
Support for real clinical decision-making
Perhaps most importantly, assessment should provide decision support, not just data. It should help clinicians determine what to target next, whether to adjust treatment intensity, and how to evolve intervention strategies over time.
When these elements are in place, assessment becomes more than a requirement, it becomes a roadmap for progress.

Expert Insights: The Evolving Role of Assessment
Improving individual assessments alone isn’t enough. What’s needed is a more comprehensive approach that connects measurement, intervention, and outcomes into a unified system.
Dr. Frazier’s work emphasizes a fundamental shift: assessment shouldn’t exist in isolation, but as an integrated component of care that informs decisions, help to guide intervention target selection, shape intervention strategy, monitor meaningful change, and inform needed care modifications as progress is observed.
Emerging frameworks like AI.Measures reflect this evolution by integrating multiple sources of data, including information about the individual patient’s profile, periodic assessments from multiple informants, and information about treatment progress. Together, these elements provide a more complete picture of the treatment journey and enable more consistent data-informed clinical decision-making.
Within this model, assessment becomes a driver of care. Baseline results inform not only what skills to target, but also treatment intensity, intervention strategy, and caregiver involvement. As care progresses, ongoing data guides adjustments, ensuring treatment remains responsive to each learner’s needs.
As expectations for accountability and measurable outcomes increase, assessment is becoming more than a clinical task, it’s a critical component of how care systems operate.
- For clinicians, structured tools that assess a wide range of skills like ABLLS-R and AFLS, combined with more advanced measurement approaches, reduce ambiguity and support more confident decision-making.
- For interdisciplinary teams, shared access to meaningful assessment data strengthens collaboration. Educators, therapists, and caregivers can align around a common understanding of a learner’s strengths, needs, and progress.
- For payors, the expectation is clear: demonstrate meaningful, measurable outcomes. Assessment approaches that support longitudinal tracking, individualized context, and transparent reporting make it easier to show that interventions are effective and justify continued services.
From Measurement to Meaningful Outcomes
Assessment has always been central to autism and IDD care, but its role is evolving. Rather than functioning as a static checkpoint, it’s becoming an integrated, ongoing aspect of care. Insights from industry leaders like Dr. Frazier remind us that assessment is more than measurement. It’s the foundation from which meaningful progress emerges.
Ultimately, better outcomes will depend not just on what’s measured, but on how effectively that information is used to guide care, demonstrate progress, and improve the lives of the individuals served.
Posted in Assessments, Clinical, Practice Management
You may also like...
Related information and stories
Guttenberg’s Interpersonal Skills Strategy: A Proactive Approach to Student Well-Being
Guttenberg Board of Education serves New Jersey students from Pre-K3 through eighth grade at Anna L. Klein School, a close-knit district built around community, belonging, and student growth. For Guttenberg…
Neurobehavioral Assessment & NASP: Rating Scales in Practice
Earlier this year in Chicago, school psychologists, clinicians, and education leaders gathered at the NASP Annual Convention to exchange ideas, debate best practices, and explore the tools shaping the future of…
CentralReach Offers Comprehensive Behavioral Health Assessment Tools and Training Resources Free to Graduate Students
Bridging the gap between the classroom and clinic, CR Assessments will provide students with the real-world tech skills needed as they begin their careers as behavior analysts. Fort Lauderdale, Fla.,…